Our services
These services are aimed at any team or organization working in the field of healthcare and social services and planning or implementing change. They may also be offered, depending on the purpose of your request, if you are involved in research or if you are a citizen.
Raising awareness and providing guidance on one dimension of change:
- Clarify the change, its scope, its importance, its impact on practice
- Plan a change and its stages
- Implementing change and its challenges
- Involve stakeholders in change
- Assessing the impact of change
- Mobilize knowledge (synthesize knowledge, identify barriers and facilitators, disseminate and implement innovations)
- Scaling up an innovation
- Support the use of a systematic approach and the co-creation of decision-support tools, as well as their dissemination
- Support for the use of the PADA tool to create decision-support tools.
- Identification and mobilization of resources to support changes in care and service trajectories in the healthcare network.
- Examples: Practice facilitators
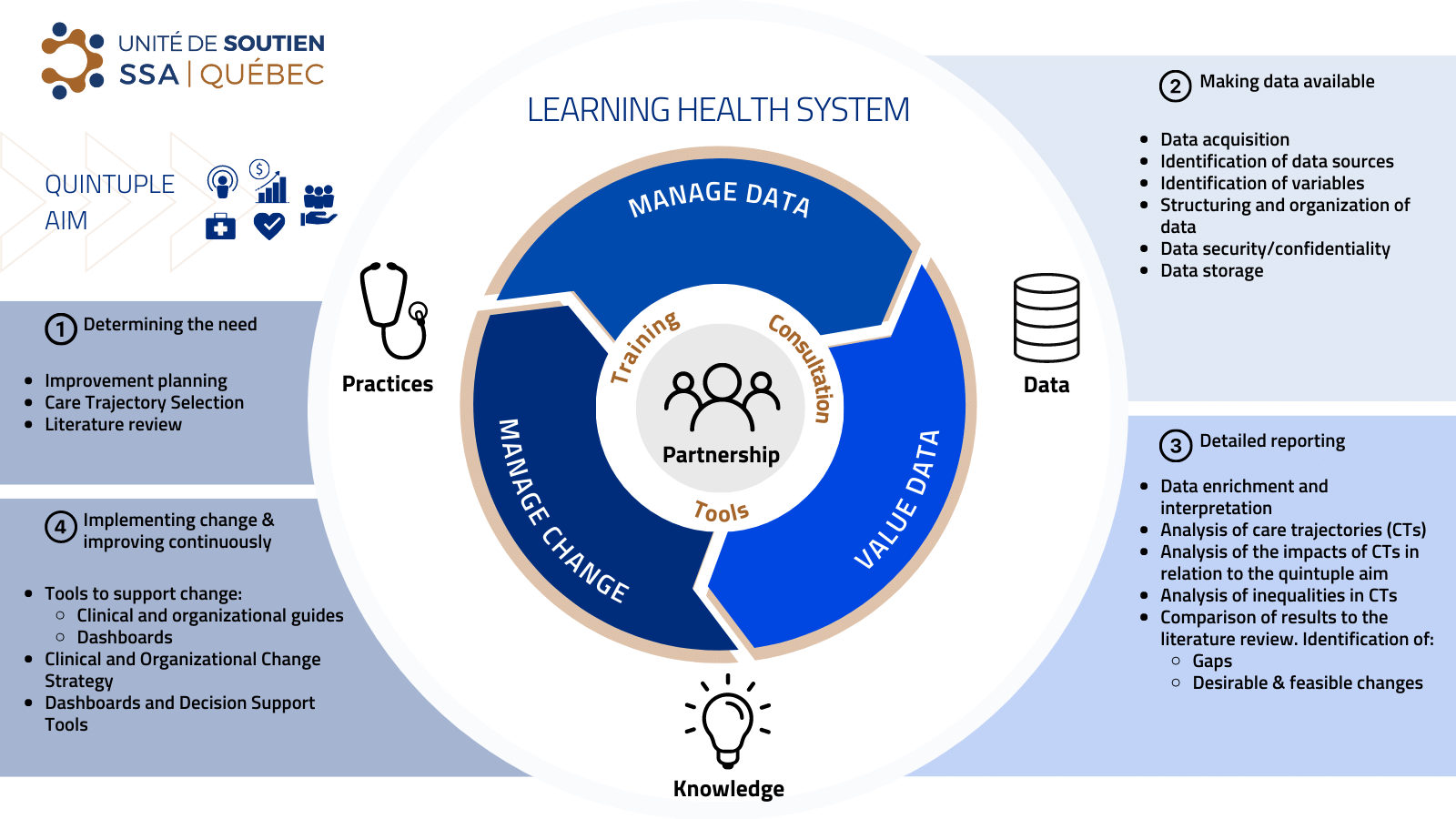
What is an LHS?
A learning health system helps us put science into our practices. It helps us measure, analyze, apply, and then repeat the cycle. From practices to data, from data to knowledge, from knowledge to clinical and organizational practices.
In a learning health system, all forces come together to eliminate working in isolation. There is a partnership between:
- Research
- Health care
- Social services
- Management
- The Public
To ensure that people receive the right services, at the right time, in the right place, with the right staff for their condition. This is called improving care trajectories. These trajectories should be as easy to follow as a recipe.
The demonstration project: an example of a learning health system
Project: Improve the ability to identify patients at risk of becoming frequent users of emergency services.
Begun in 2016, in support of the V1SAGES program, this flagship project helped demonstrate the value and benefits of the learning health system (LHS) approach. Led by an interprofessional team involving patients and their loved ones, it embodied a research continuum, from structured data collection and expansion of its use, to producing tools to support decision-making and, ultimately, integrating the knowledge acquired into clinical and organizational practices.
Three streams and objectives
- Improve the ability to identify patients at risk of becoming high utilizers of emergency departments;
- Further integrate the social and community dimension with the health dimension;
- Identify the decision-making issues of individuals who are heavy users of services and have complex needs.
Features
- Multidisciplinary and interprofessional team;
- Active involvement of six patient partners in all phases of the project;
- Support from most of the resources of the Unit’s team
Process
- Systematic review, data collection on decision-making needs and modalities of integration of health and social dimensions;
- Development and validation of clinical tools.
- Development of the CONECT-6 tool, a tool for identifying individuals at risk of becoming heavy users of emergency services, and its implementation in clinics;
- Enhanced training for clinical staff;
- Optimization of the role of nurses in the follow-up of clients with complex needs and at risk of becoming high users of emergency services.
As part of the demonstration project, we provided POR capacity-building support to six patient partners, three researchers, six professional research staff members and ten members of the student community.
To this day, all of these people work in the POR field. This had a leverage effect, as several of them subsequently received training or career grants and substantial funding, including:
- A $4 million grant over four years to implement a case management intervention based on the V1SAGES program model in ten primary care clinics in five Canadian provinces;
- A $575K grant from the MSSS Targeted Granting Program in partnership with the Unit and the FRQ-S;
- Continuation of the demonstration project. The team is working on the development of a series of online training sessions for clinical teams. In addition, it is aiming to scale up the V1SAGES approach to other clinical institutions in Québec.
- Learning resulting from a multicentric study: a new article by Marie-Eve Poitras and her team as part of the Unité de soutien SRAP du Québec demonstration project
- New shared-decision aid for high users of health care services and their care teams
- CONECT-6: the first case-finding tool to rapidly identify patients suffering from chronic disease with complex health needs
Julie Godbout, Nurse, V1SAGES team case manager
Being a case manager has radically changed my relationship with clients. I used to see myself a bit like a teacher who provided knowledge to patients who just had to follow my advice and recommendations, because it was the right thing to do to be healthy! […] Now, I see myself as a resource, partner and coach.
Of course we have knowledge to pass on to patients, but they are ultimately responsible for making decisions about their lives and health. […] The case manager is there to support them, offer services, help them make decisions and navigate the health care system. They allow for a more thorough assessment of the individual’s needs.
Case management has also allowed me to develop relationships with other professionals and community resources, to better understand their roles and when and how to contact them when needed.
[…] Now when they have a patient with complex needs or a difficult situation, their instinct is to talk to other professionals. A co-development group was even set up to provide a forum to discuss these situations. Concrete solutions and concerted actions have emerged. Now that I’m replacing people in other fields, I miss these meetings.
News
See allNearly $6 million to continually improve services for young people in Québec
The Unité de soutien SSA Québec develops the GMF apprenant program
Mr. Kenneth George, patient partner, passes away
Quebecers believe that the well-being of health care teams and science should guide health care decisions above all else
Deliverables and tools
See allDecision Aid for Colorectal Cancer Screening
PADA: a Collaborative Digital Platform for Authors of Healthcare Decision Aids
An infographic summarizes how to activate Québec's learning healthcare system
Find out what's a learning health system in 60 seconds
Publications
See allInforming the development of the SUCCEED reporting guideline for studies on the scaling of health interventions: A systematic review
An infographic summarizes how to activate Québec's learning healthcare system
The Unit contributed to the Portrait sur les politiques publiques de l’Observatoire des tout-petits
How to meaningfully and equitably involve patients and the public in scaling up: upcoming publication of a study protocol
Videos
See allFind out what's a learning health system in 60 seconds
Écosanté: enhancing knowledge, competencies and collaboration opportunities related to health economics
Themes
See allQuébec's health system
Service request
When you apply for support from the Unité de soutien SSA Québec, you are taking part in the emergence of a learning health system (LHS). We offer three types of support: training, consultation and tools.
Team
Claude Bernard-Uwizeye
Coordination – Change Management (Université Laval branch)
Vanessa Fayolle
Coordination – Change Management (HEC branch)
Find out more about our
Denis Chênevert
Scientific Comanagement – Axis Change Management (HEC branch)
Find out more about our Implementation and change management expertise
France Légaré
Scientific Comanagement – Axis Change Management (ULaval branch)
Yves Couturier
Accès Recherche portal
Newsletter
Subscribe! A benchmark for Quebec’s Learning Health System.